Chronic myeloid leukemia with soft tissue infiltration: a case report
Teks penuh
Gambar
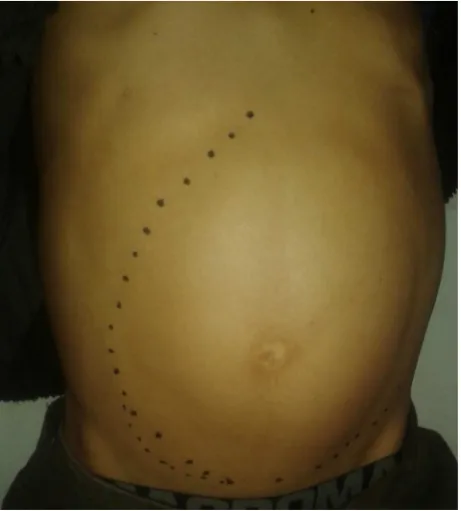
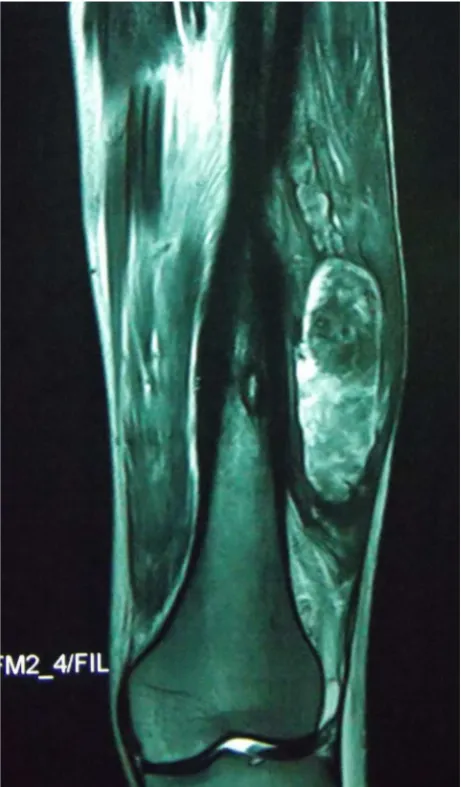
Dokumen terkait
Ini berarti bahwa penggunaan model Advance Organizer berbantu animasi komputer adalah efektif digunakan dalam melihat hasil belajar fisika siswa SMA Rambah Hilir baik
[r]
Bahwa kemudian esok harinya tanggal 04 Pebruari 2013 ibu Termohon datang kerumah Pemohon atas sms Pemohon maka Pemohon menyampaikan kepada ibu Termohon
Visa tinggal terbatas bagi pelajar /mahasiswa asing dalam rangka mengikuti pendidikan diindonesia, dapat diberikan untuk jangka waktu izin tinggal terbatas selama 5 (lima)
Apa Saja, Bagaimana Prinsip dan Konsep Desain Software...2.1 Penjelasan Tentang Metode Desain Perangkat Lunak...2.2 Pendekatan Yang Digunakan Dalam Desain...2.3 Manajemen
Pandangan yang sama turut dinyatakan oleh Abdul Basit (2014) yang menjelaskan bahawa kesenian boleh digarap sebagai media dakwah yang menepati uslub-uslub dakwah
Pembangunan sistem pendukung keputusan menggunakan Multi Factor Evaluation Proces dapat dilakukan melalui pengkodean menggunakan bahasa pemrograman berbasis
dan dengan voltase yang lebih rendah dari output dioda, maka dapat ditambahkan. rangkaian stabilisasi tegangan berikut