Anatomic Reconstruction Of The Distal Radio-Ulnar Ligament and Osteotomy For Malunion Distal Radius and Ulna With Distal Radio-Ulnar Joint Instability.
Teks penuh
Gambar
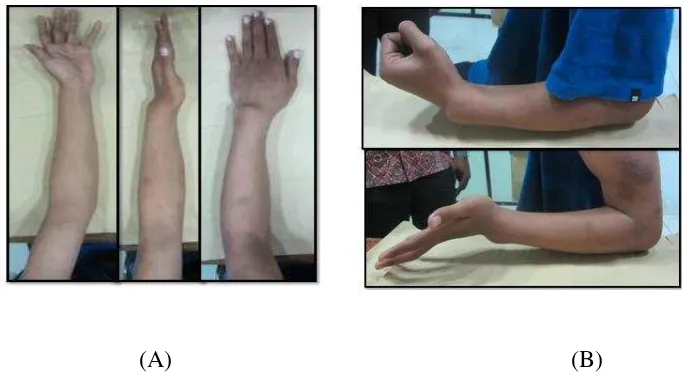
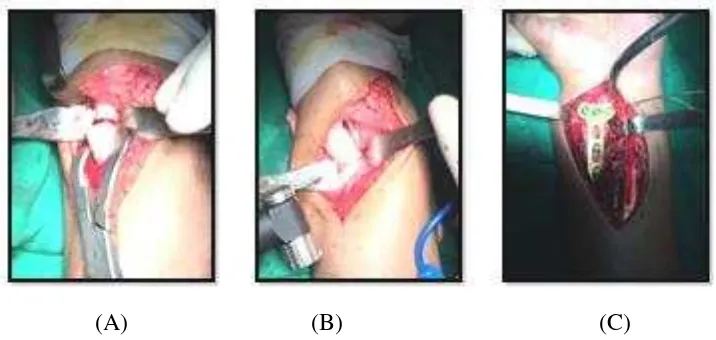
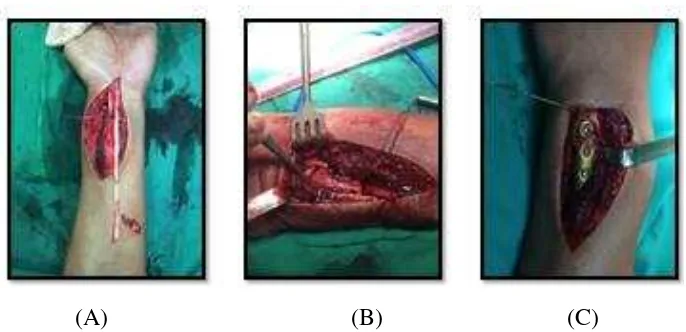
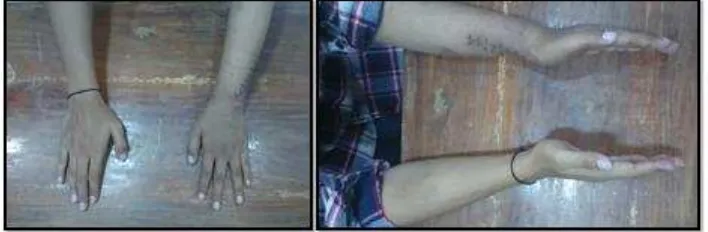
Dokumen terkait
Dalam Bahan Ajar ini anda akan mempelajari kompetensi dasar Perwajahan serta memperhatikan dasar-dasar pokok perwajahan serta membuat desain secara manual sebagai salah
[r]
Hasil Evaluasi Adminitrasi : Memenuhi Syarat Hasil Evaluasi Teknis : Memenuhi Syarat Hasil Evaluasi Harga/Biaya : Memenuhi Syarat Hasil Evaluasi Kualifikasi : Memenuhi Syarat.
Ainsi, dans le cadre d’une société spéctacularisée marquée par un shopping de plus en plus thématisé, la fréquentation d’un magasin populaire comme Babou, Tati ou Gifi devient
Pada hari ini Selasa tanggal Dua Puluh Lima bulan September Tahun Dua Ribu Dua Belas, kami yang bertanda tangan dibawah ini Panitia Pengadaan Barang dan Jasa Dinas Bina Marga
Menggunakan metode tersebut, selain sesuai dengan pelaksanaan pendidikan vokasional yang dilaksanakan di Lapas Kelas II A Kutoarjo, hal tersebut juga mempermudah
Setelah diumumkannya Pemenang dalam Pelelangan ini, maka kepada Peserta yang berkeberatan/ berkepentingan atas pengumuman dimaksud dapat menyampaikan sanggahan secara
It is increasingly likely that developing countries in the Asia-Paciic region will incorporate forest-related activities into inancing strategies for climate change