Volume No.: 1 Month: December Issue: 3 First page No.: 196 P-ISSN.2503-0817 E-ISSN.2503-0825 http:dx.doi.org10.15562jdmfs.v1i3.317 Case Report
Teks penuh
Gambar
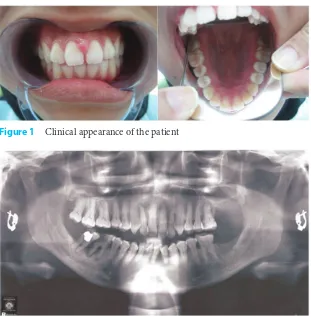
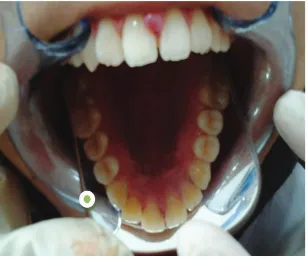
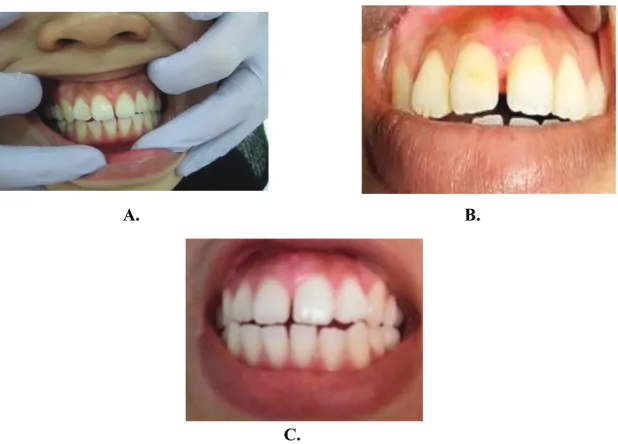

Dokumen terkait
e) Persepsi Individu.. Available Online: https://dinastirev.org/JMPIS Page 341 Penugasan secara individual yang diberikan oleh pimpinan, dimana individu merasa
Abstrak: Proses produksi yang diterapkan oleh sebuah perusahaan manufaktur dalam industri 4.0 saat ini, tidak terlepas dari penggunaan sistem informasi
Fisioterapi: Cegah komplikasi atrofi dengan melakukan peregangan pada otot yang spastik (stretching), latih kekuatan otot secara pasif dan aktif (strengthening) Ajar latihan
Dengan demikian dapat disimpulkan bahwa pengendalian internal bukan sebagai variabel pemoderasi bagi pengaruh peran auditor internal terhadap kinerja organisasi
Oleh karenanya pencermatan terhadap Surat Dakwaan, Nota Keberatan, Alat Bukti dan segala sesuatu yang terungkap serta terbukti di pèrsidangan, Surat Tuntutan
Selanjutnya hasil penelitian ini sejalan dengan penelitian yang dilakukan oleh Purnama (2016). Dimana hasil analisis yang diperoleh secara parsial menunjukkan bahwa
Jurnal Konseling Andi Matappa Volume 4 Nomor 1 Februari 2020 Hal 28 34 p ISSN 2549 1857; e ISSN 2549 4279 (Diterima Oktober 2019; direvisi Desember 2019; dipublikasikan Februari 2020)
Persentase yang diperoleh dari hasil Faktor yang melatar-belakangi tingkat akurasi dan atau tidak akurasinya penilaian yang dilakukan oleh pada dosen terhadap praktik PKP dan