FULL PAPER
THERAPEUTIC RESPONSE EVALUATION ON
HYPERTHYROIDISM USING A FIXED DOSED OF I-131
Yulia Kurniawati, and
AHS Kartamihardja
Department of Nuclear Medicine, Dr. Hasan Sadikin General Hospital,
Faculty of medicine Universitas Padjadjaran,
Bandung, Indonesia
POSTER PRESENTATION
4
thInternational Conference on Radiopharmaceutical Therapy
New World Hotel, Ho Chi Minh City, Vietnam
THERAPEUTIC RESPONSE EVALUATION ON
HYPERTHYROIDISM USING A FIXED DOSED OF I-131
Yulia Kurniawati, and AHS Kartamihardja
Department of Nuclear Medicine, Dr. Hasan Sadikin General Hospital, Faculty of Medicine Universitas Padjadjaran,
Bandung, Indonesia Abstract
Introduction.Euthyroidism condition is the ideal expected after treatment of
hyperthyroidism, but there is still no established therapeutical method that can achieve that condition. Radioactive iodine-131 (131I) has been used to treat hyperthyroidism for long time. It is clinically effective, safe, and cost-effective. However, controversy over the optimum dose of I-131 therapy is still debatable. The aim of this study was to evaluate the therapeutic response of a fixed dosed I-131 in hyperthyroidism patients.
Material and method. Retrospective study was carried out during January 2010 until January of 2011. The inclusion criteria were all subjects received I-131 for the first time with a fixed dose of 8 mCi, diffused and high uptake of Tc-99m. Theraupeutical response was evaluated based on the patient’s clinical state and or their laboratory finding3 months after the treatment. Theurapeutical response categorizedgood response if thyroid hormones within normal limit and/or improvement of clinical state, when thyroid hormones still high (above normal value ) with improvement of clinical state was considered as partial response, no respons if there was no changes both on laboratory finding and clinical state.
Results. There were 127 patients receiving a fixed dose I-131 therapy of 8 mCi during
32(36,78%) were no response, still considered in a hyperthyroid condition, 55 (63.21%) patients have good responses, which were20 (36.36%) were hypothyroid, 21 (38.18%) were euthyroid and 14 (25.45%) were partial responses.
Conclusion.Fixed dose I-131 therapyof 8 mCi showed good response in our hospital on
hyperthyroidism, thereforewe can considered as dose of treatment.
Introduction
Hyperthyroidism is a hypermetabolic condition with increased thyroid hormone production.1,2 Study based on community showed that the incidence of hyperthyroidism found more in female than male. The prevalence of hyperthyroidism was about 2 % in female and 0,2% in male.3 A study conducted in UK involving 2.779 people with mean age was 58 years old showed the incidence of hyperthyroid was 0,8 per 1.000 female per year.4
The objective of hyperthyroidism treatment is to restore thyroid hormone level to normal range or euthyroidism.5 Euthyroidism can be achieved by destroyed thyroid tissue or inhibite synthesis and release of thyroid hormone.1 Destroying thyroid tissue could be done by surgery or radioiodine ablation and inhibition of synthesis and release thyroid hormone can be achieved by oral antithyroid drug.1, 2, 6, 7
Recurence hyperthyroid was observed in 34% patients treated with oral anti thyroid drug. This is the highest among the other treatment modalities. Recurrence hyperthyroidism after treatment by using I-131 ablation and surgery were 21% and 8% respectively.8 I-131 now is considered to be drug of choice or second linetreatment after oral antithyroid drugfor hyperthyroidism patients. However, the optimum dose of
hyperthyroidism. The dose of I-131 could be given as fixed dose 5-15 mCi based on empirical study or calculated dose.7,9,10Calculated dose usually depend on weight of thyroid gland and I-131 uptake ability of thyroid gland.10,11 The aim of this study was to evaluate the therapeutic response of a fixed dosed I-131 in hyperthyroidism patients.
Material and method
Retrospective study was carried out during January 2010 until January of 2011 in Department of Nuclear Medicine, Dr. Hasan Sadikin General Hospital. Hyperthyroidism patient with diffuse and high uptake thyroid on 99mTc- pertechnetate thyroid scintigraphy were included in this study. Subject was received a single fixed dose of 8 mCi I-131 for the first time. Therapeutical response was evaluated based on
the patient’s clinical state and or their laboratory finding 3 months after the treatment.
Theurapeutical response categorized as good response is considered if thyroid hormones within normal limit and/or improvement of clinical state, when thyroid hormones still high (above normal value) with improvement of clinical state was considered as partial response, and no respons if there was no changes both on laboratory finding and clinical state.
Results
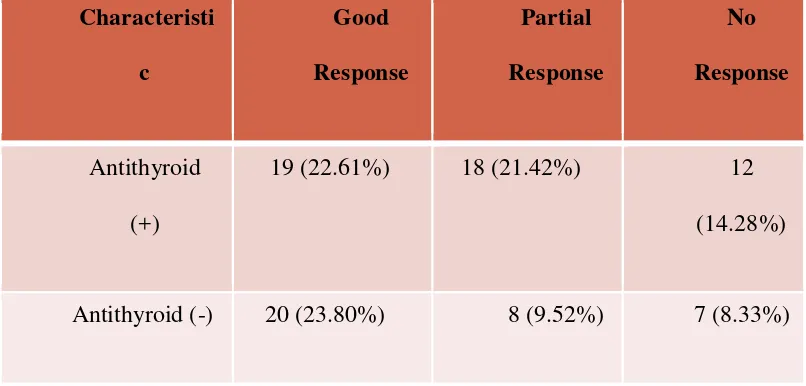
to radioiodine ablation was 49 (58.33%) and rest of them had no history of taking antithyroid drug. From the 84 patients, 39 (46.42%) subjects showed good responses, 26 (30.95%) were partial response and 19 (22.61%) were no response. Among subject with good and partial response (65 subject), there were 20 (36.36%) developed hypothyroidism, 21 (38.18%) were euthyroid and 14 (25.45%) were partial responses.
Table 1. Therapeutic response based on history of antithyroid drug (n=84) Characteristi female subject (67.85%) was more than male in this study.
Controversy on the use of I-131 for treatment of patient with hyperthyroidism is
not only on the issue who will take advantages of this treatment as first line or second
line, but also there is no established protocol on dose given to the patient. Some
clinicians believe that the goal of radioiodine ablation is to achieve euthyroidism status
as soon as possible and maintain this status as long as possible before come to
hypothyroidism. This group of clinicians usually will give lower dose, bus as
groups of clinicians believe that all hyperthyroidism patients, particularly grave’s
disease will end with hypothyroidism and the management of hypothyroidism is more
simple and less complication. Due to these reasons, the goal of radioiodine ablation is
to reach hypothyroidism status by using high dose of I-131.5,7
Theoritically, calculated dose is the best choice to treat hyperthyroid, but in fact
calculated dose applied in many department based on weight and thyroid uptatke was
not sufficient. This condition due to the effetiveness of I-131 on hyperthyroid patients
was also influenced by many factors such age, gender, ethnic and history of smoking.
Anti thyroid drug taken prior to radioiodine therapy also could interferen the efficacy of
treatment.1 Due to this situation many center of nuclear medicine used fixed dose of
I-131 ranged 8-15 mCi.1,5,12,13,14
The result from this study showed good and partial response was obseved in 55 (65.47%) subjects. Similar study was done in Bangladesh using fixed dose 8-15 mCi and the result was 82%,15 This better results could be due to several patients were recieved higher dose from 8 mCi. The higher the dose of I-131, the faster the hypothyroidism achieved.1,14 This result was support by other study done in India. The
effectiveness of radioiodine ablation using fixed dose of 5 mCi was less than 59,37%
Subject with history of taking antithyroid drug prior to radioiodine ablation was 49 (58.33%) and rest of them had no history of taking antithyroid drug.1 Although the impact of preceding antithyroid drug on the outcome of I131 is still debatable, our data suggest that the drug can reduces the therapeutic efficacy.
Conclusion
Fixed dose I-131 therapy of 8 mCi showed good response in 3 month follow up for the treatment of hyperthyroidism. Anti thyroid drugs may be a factor that can reduces efficacy of I-131 on the treatmen of hyperthyroidism.
Referrences
1. Meier. DA, Dworkin. HJ, Bender. JM. Therapy for Hyperthyroidism. In: Henkin. RE, Bova. D, Dillehay. GL, Halama. JR, Karesh SM, Wagner RH, et al., editors. Nuclear Medicine. 2nd ed. Pennsylvania: MOSBY elsevier; 2006. p. 1567-75 2. Cooper. DS, Greenspans. FS, Gardner. DG, Ladenson. PW. The Thyroid Gland.
Basic & Clinical Endocrinology. 7th ed. New York: McGraw-Hill; 2004. p. 209-78.
3. Reid JR, Wheeler SF. Hyperthyroidism: diagnosis and treatment. Am Fam Physician. 2005 Aug 15;72(4):623-30.
4. Vanderpump MP, Tunbridge WM, French JM, Appleton D, Bates D, Clark F, et al. The incidence of thyroid disorders in the community: a twenty-year follow-up of the Whickham Survey. Clin Endocrinol (Oxf). 1995 Jul;43(1):55-68.
6. Jamerson. JL, Weetman. AP. Disorders of The Thyroid Gland. In: Kasper. DL, Braunwald. E, Fauci. AS, Hauser. SL, Longo. DL, Jamerson. JL, editors. Harisson's Principles of Internal Medicine. 16th ed. New York: McGraw-Hill; 2005. p. 2113-7.
7. Weetman AP. Graves' disease. N Engl J Med. 2000 Oct 26;343(17):1236-48. 8. Torring O, Tallstedt L, Wallin G, Lundell G, Ljunggren JG, Taube A, et al. Graves'
hyperthyroidism: treatment with antithyroid drugs, surgery, or radioiodine--a prospective, randomized study. Thyroid Study Group. J Clin Endocrinol Metab. 1996 Aug;81(8):2986-93.
9. Klein I, Becker DV, Levey GS. Treatment of hyperthyroid disease. Ann Intern Med. 1994 Aug 15;121(4):281-8.
10.Iagaru A, McDougall IR. Treatment of thyrotoxicosis. J Nucl Med. 2007 Mar;48(3):379-89
11.Leslie WD, Ward L, Salamon EA, Ludwig S, Rowe RC, Cowden EA. A randomized comparison of radioiodine doses in Graves' hyperthyroidism. J Clin Endocrinol Metab. 2003 Mar;88(3):978-83
12.Moore. KL, Dalley. AF. Neck. Clinically Oriented Anatomy. 5th ed. Baltimore: Lippincott Williams & Wilkins; 2006. p. 1083-7.
13.Singer PA, Cooper DS, Levy EG, Ladenson PW, Braverman LE, Daniels G, et al. Treatment guidelines for patients with hyperthyroidism and hypothyroidism. Standards of Care Committee, American Thyroid Association. JAMA. 1995 Mar 8;273(10):808-12.
Deficiency Goiter Belt in the Himalayan Valley of Kashmir, India. World J Nucl Med. 2006;5:109-14.