94 Ghalaut et al. Med J Indones
A
study of
oral
glucose
tolerance
test
in preeclampsia
Veena Singh Ghalaut*,
Nirmal Gulati**,
PartapSingh Ghalautt,
Simmi
Kharb*
Abstrak
Kehamilan akan merangsang resistensi insulin yang mengakibatkan terganggunya metabolisme karbohidrat dan meningkatnya kejadian preeklampsia-eklampsia. Terdapat pula peningkatan morbiditas dan mortalitas janin. Penelitian ini dilakulan pada 25 kasus preeklampsia ringan, 25 knsus preeklampsia berat, dan 50 wanita hamil normotensif yang sesuai umur, paritas dan usia gestasinya. Pemeriksaan klinik lengkap termasuk pemeriksaan Hb, urin lengkap, ureum darah, asam ura4 kreatinin, dan toleransi glukasa oral dilakulcnn.Terdapatkenaikanbermalmadalammortalitas danmorbilins perinatalpadapreeHampsiaberat. Hipoglilæmialebihbanyak diternukan pada preeklampsia berat dan hiperglikemia pada preeklampsia ringan. Pemeriksaan glukosa darah penting dalam meramallean keadaan janin pada kasus-lcasus tersebut.
Abstract
Pregnancy induces
a
stateof
insulin resistance leading to disnrbed carbohydrate metabolism and increased incidenceof
preeclampsia-eclampsia. There is increased incidence of fetal morbidity and mornlity. The present study was canied out in 25 mild preeclamptic woman, 25 severe preeclamptic woman and 50 age,
paity
and gestation matchednormotensive pregnant women. Thorough clinical examinationwas done and hemoglobin, urtne complete examinarton, blood urea, serum uric acid, creatinine and oral glucose tolerance were estimated. There is significant increase inperinatal mortality and morbidity in severe preeclampsia. Hypoglycaemiawas more cotnmonly seen in severe preeclampsia and hyperglycaemia in mild preeclampsia. Hence, blood glucose estimation is important to predict the fetal outcome in such patients.Keywords: gestational diabetes, pertnatul mortality, preterm deliveries, birth asphyxia
INTRODUCTION
Preeclampsiais
acommon
occurrence in diabeticpreg-nancy
and a causeof perinatal
mortality. During
preg-nancyfasting blood
glucose levelsfall
due to increasedlevels
of insulin.l'2
This
responseis
dueto
pregnancyinduced
stateof
peripheral
resistance toinsulin
due to increasedlevels
of
estrogen and progesterone, humanplacental
lactogen
and
insulinase activity
of
placen-ta.''*
lnconclusive literature
is
available
on
car-bohydrate metabolism
in
preeclampsia. Burt5
showed a consistentimpairment
of carbohydrate tolerancewith
relative hyperglycaemia
and
decreasedsensitivity
to
exogenousinsulin in
preeclampsia
and decreasedsen-sitivity
to exogenousinsulin
in
preeclampsiawhich
heattributed to defective hepatic
storageof
carbohydrate leading tohyperglycaemia.
The present study has been* Department of Biochemistry,
**
Department of Medicine,f
Department of Obstetrics and Gynaecology,Pt. B.D. Sharma PGIMS, Rohtak-124001, Haryana, India
carried
out for
abetter understanding
of
carbohydraemetabolism
in
preeclampsia
andrelation
of
abnormal
glucoselevels
with
perinatal
outcome.MATERIALS
AND
METIIODS
One hundred patients
in
last
trimester
(28-40
weeks)of
pregnancy admitted/attending antenatal
clinics
of
Pt. BDS, PGIMS,
Rohtak,
India were
studied
in two
groups.
Group
I
subdivided
as
group 1A having
25patients
with
severe
preeclampsia
(diastolic blood
pressure>
110mmHg, albuminuria > 2+)
andgroup
18 having
25 patients
with mild
preeclampsia
(dias-tolic
blood
pressure
<
110 mmHg, albuminuria
of
Vol7, No 2,
April
- June 1998glucose was
estimated by glucose
oxidase peroxidasemethod./
RESULTS
The levels
of
blood urea and serum
uric
acid
weresignificantly higher
in
severepreeclampsia as
com-pared
to mild
preeclampsia
(p
<
0.01
in
both
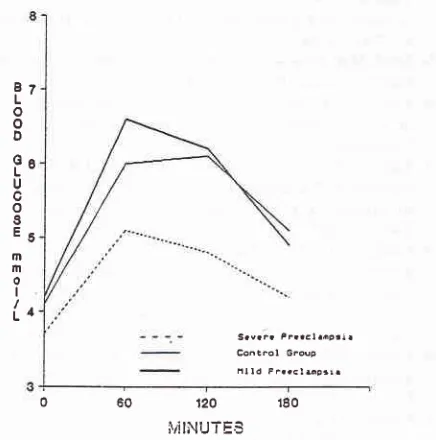
the parameters).The mean fasting, one hour and two hour blood sugar
levels in
severepreeclampsia
weresignificantly lower
as compared
to
control
(p <
0.05) as
well
as mild
preeclampsia
(p <
0.05). There was
no
statistically
significant
increase in fasting and one hour blood sugarin mild
preeclampsia
as comparedto control.
2nd
and3rd hour values
'were
almost equal
in
mild
preeclampsia
and control (Figure 1).0
60
120
180ùiINUTES
Figure 1. Blood glucose curtte in study and control group
Incidence
ofhyperglycaemia in mild preeclampsia was
24Vo and
in
severe preeclampsia
was 6Vo whereasin-cidence
of
hypoglycaemia
in
mild
preeclampsia
was 4Vo and severepreeclampsiawas
8Vo.There
were
15preterm
and l0 term deliveriesin
severe preeclampsia.While in mild preeclampsia
andcontrol group
majority
of
patients
delivered at term and
only 6 patients
eachhad
preterm
delivery. (Table
1) Meanbirth weight
of
term
babies
of
hyperglycaemic patients was
sig-nificantly
higher
as compared to normoglycaemic andhypoglycaemic patients
in
study group
(p
<
0.001,Table
2). Five
babies
were large
for
date
in
mild
preeclampsia
ascompared to four in control and none
in
severepreeclampsia.
Oral glucose tolerance test in preeclampsia
Table l. Neonatal complications in study and control group
No. of cases
Complications
Group
1A
GrouplB
Group 2 95Preterm
(Mean birth weight, g) Term
(Mean birth weight, g)
Birth asphyxia
Hyperbilirubinemia
Hypoxia
Congenital malformation
Perinatal mortality: Still birth First week death
15 (1600) 6
(1800)
6 (1e00)l0
(2400)
19(2800)
44(32OO)ll
4
4965
t40
002
4
(t6Vo)
|(4Eo)
I (2Vo)3
(t2Eo)
I(4Vo)
3 (6Vo)Table
2.
Effect of abnormal glucose tolerance on mean birth weight in various groups (g, mean + SD)i?
o o
D
fe
Uc o s E5
m
m
o
I
{.t
Groups
Number
Birthweight
Birth weight inhypergly-
inhypogly-caemics
caemicsBirth weight in
normogly-caemla
2
1500-+0.4
l600m.52500È0.4
250O10.3160010.3
2000i0.82600t0.8
300G,r0.4Group
I
Hyperglycaemics Vs. Normoglycaemics p value < 0.001Group
I
vs 2 (Normoglycaemics) - p value < 0.001DISCUSSION
In
present stady 78Vo
of
preeclamptic women
had edema feet as comparedto
22Voin normotensive
con-trol. Thomsonu reported
edemain
85Voof preeclamptic
and 40Vonormotensive pregnant.
Serumuric acid was
significantly higher
in
severepreeclampsia
(0.034,t
0.6 mmoUl)
as comparedto mild preeclampsi
a(0.021
+
6mmol/l),
(p < 0.01).Mean fasting blood
glucosein
severe preeclampsia
(3.7
+ 0.5 mmol/l)
was
sig-nificantly
lower
as compared tomild preeclampsia(4.2
+
0.8 mmol/l), (p < 0.5).Our
findings are comparable
to those
of
Singhe
andYamamotoru;
where mean values were 3.3, 3.6mmol/l
respectively.
All
the postprandial values
in
severepreeclampsia were significantly lower
as comparedto
control (p
<
0.001). Whereas
in
mild
preeclampsia,first
hour post prandial value
was higher than controland
second
hour values were similar in mild
Preterm Term Preterm
Term
2200LO.3 350O:ù0.7
340010.6
l5
l0
6 44
S.e.F. PF..<1.ôp.i. ConÈ.ol 6Foup
[image:2.595.300.536.117.501.2] [image:2.595.50.268.311.531.2]96 Ghalaut et al.
preeclampsia and
control.
Similar
observations
were madeby
îallarigo.ll
Incidence
of
hyperglycaemia
andhypoglycaemia
wassignificantly higher
in
the
study groups.
In
severepreeclampsia
44Vohad
hypoglycaemia
and 56Vohad
normoglycaemia. Whereas
Longl2
found
hypo-glycaemia
in
22.3Voof
cases andhyperglycaemia
and4Vo
had hypoglycaemia and
rest
were
normo-glycaemic.
Thesefindings
are consistentwith
thoseof
Yamamoto.l0 lncidence
of
gestational diabetes in
study andcontrol groups
was 6Vo and4Vorespectively.
Singh' reported
26.7Vo
incidence
of
gestational
diabetes
which he attributed
to
anoxia
of
B-cells
in
preeclampsia.
According
to
Longl2
abnormal
glucosetolerance
is
more
likely to
precede
the
onset
of
preeclampsia than to
be a consequenceof it.
Reducedmaternal
supply
of
nutrients
to
the
fetus
may be
the causeof preeclampsia
asfetal growth retardation often
precedes
the
appearanceof
the
signsof
preeclampsia.In
severepreeclampsia
with
hypoglycaemia incidence
of
prematurity was significantly higher
(60Vo) more
often
in
hypoglycaemics.
Mean birth weight
of
term
babies
of
severepreeclampsia
wassignificantly lower
thanmild
preeclampsia
andcontrol. It
was alsofound
that
mean
birth
weight
in
hyperglycaemics
was
sig-nificantly
higher
thannormoglycaemics both
in
study andcontrol groups.
No
large for
datebaby
was seenin
hypoglycaemics
while 5
patients
with
mild
preeclampsia
and
four
normotensive
control
hadlarge
for
date babies. Various
studies
have similar
results.ll'14-17Hypoglycaemia was more
common
in severe
preeclampsia
while
hyperglycaemia was
seenin mild
preeclampsia. Fetpl
morbidity
andmortality
was
sig-nificantly
increased
in
preeclamptic women
with
ab-normal blood
glucose
levels
and hypoglycaemia
hadomnious
significance with
regardsto
perinatal
death.Blood
glucose
analysismay
serveto predict fetal
out-come
in
casesof
preeclampsia.Med J Indones
REFERENCES
l.
Lind T. Metabolic changes in pregnancy relevant to diabetesmellitus. Post Grad Med J 1979;55:353-60.
2. Spellacy
WN,
Goetz FC. Plasma insulinin
normal late pregnancy. New Engl J Med 1963;268:988-97.3. Baumann G, Puavilai G, Freinkel N, Domout LA, Metzger BE, Levene HB. Hepatic insulin ând glucagon receptors in pregnancy, their role in enhanced catabolism during fasting. Endocrinol 1981 ;108: 1979.
4. Freinkel N. Banting Lecture 1980 of pregnancy and progeny. Diabetes 1980;29 :1.023.
5. Burt RL. Peripheral utilization of glucose in pregnancy and
preeclampsia. Obstet Gynecol 1955;6:5 1-4.
6. O'Sullivan JB, Mahan CM, Charles D, Dandroo RV.
Medi-cal
Treatmentof
gestational diabetes. Obstet Gynecol 1974;43:817-21.7. Maclanchar
DM.
Glucose, other sugars and ketones. In: Gowenlock AN ed. Practical clinical Biochemistry. 6th ed.Great Britain ; Heineman professional publishing I 988 ;3
20-2.
8. Thomson AM, Hytten RE, Billewicz Vy'Z. The epidemiology of edema during pregnancy. J Obstet Gynec
Br
Common wealth l97I;78:520-9.9. Singh MM. Carbohydrate metabolism in preeclampsia. Br J
Obstet Gynecol l9'l 6;83 :124-3
l.
1 0. Yamamoto K. Studies of plasma insulin in women and effect
of
glucose administrationin
toxemiaof
late pregnancy. Tokushima J Exp Med 1967;14:91-106.11. Tallarigo L, Giampetro O, Penno G, Miceoli R, Gregori G,
Navalesi R. Relation of glucose tolerance in complications
of
pregnancyin non-diabetic women.
N
Engl
J
Med1986;3 l5:989-92.
12. Long PA, Abell DA, Beischer NA. Importance of abnormal glucose tolerance (hypoglycaemia and hyperglycaemia) in aetiology of preeclampsia. Lancet 1977 ;l:923-5.
13. Singh
M, Giri
SK, RamachandranK.
Intrauterine growthcurves in live bom babies. Indian Paediatr 1974;ll:475-80.
14. Lindsay
MK,
Graves W, Klein L. The relationship of oneabnormal test value and pregnancy complications. Obstet Gynecol 1989 ;7 3 : 103 -6.
15. Campbell DM. Glucose tolerance in complicated pregnan-cies.
In:
SutherlandHW,
StowersJM
eds. Carbohydrate metabolismin
pregnancy andnewborn.
New
York:
Springer-Verlag Berlin Heidelberg 1979.'509-14
16. Long PA, Abell DA, Beischer NA. Fetal growth retardation
and preeclampsia. Br J Obstet Gynecol 1980;87:13-16. 17. Kapoor M, Aggarwal N, Jain PK, Sethi RS, Gupta U, Latika