Diagnosis Of Hookworm Infestation
By Using Modified Kato-Katz Thick Smear
Syahril Pasaribu Chairuddin P. Lubis
Department of Pediatrics Faculty of Medicine University of North Sumatera
INTRODUCTION
Intestinal nematode infections constitute a major health problem in the third world, particularly in tropical countries where optimal conditions exist for propagation of these helminths1,2,3,4,5,6,7,8.
High prevalence of the most important soil transmitted helminthiasis, Ascaris lumbricoides, Trichuris trichiura and Hookworm as well as their occurrance in multiple infections are commonly found in several areas in Indonesia9,10,11,12,13 and the infection are prominent among school children14,15.
The morbidity of hookworm infections in endemic areas is sustained primarily by children. In one study half of the children were infected before age 5; 90% were infected by 9 yr of age. Intensity of the infection increases up to age 6-7, then stabilizes for a few years16.
The diagnostic methods for hookworms and related nematode infections by the recovery of larvae from faecal samples have various advantage over the conventional diagnostic methods of the examine of parasite eggs in faeces. The culture methods are more snsitive and efficient for detection of the infection than direct examination of eggs in faeces, because the amount of faecal samples being examined is much larger; in routine faecal examinations, some 10 mg or less is examined in direct faecal smear method, some 50 mg in thick faecal smear method, but some 500 mg of faecal samples can be examined by using the test tube method and much more samples can be cultured in the polyethylene tube method17,18.
MATERIALS AND METHODS
This study had been done as a double blind study from January - March 1996. Stool samples of 541 children from two primary school in the rural areas of North Sumatera Province were examined to determine the infection rates of soil transmitted helminthiasis.
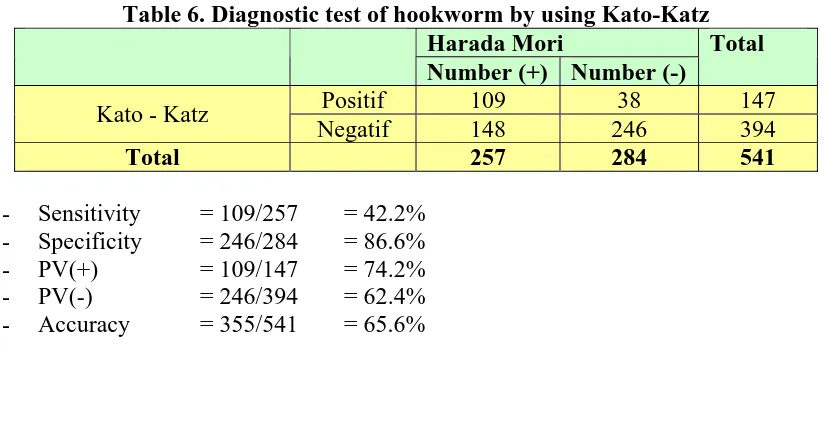
Every stool samples were examined by using a modified Kato-Katz thick smear and a modified Harada-Mori technique.
Data analysis comprises: gender, age, nutritional status, occupation of the father, educational level of the parents.
RESULTS AND DISCUSSIONS
From 541 stool samples, we found that 469 of them were positive (86.7%). with eggs or larvae. Mixed infestations were 374 (79.7%) and 95 (20.3%) was single infestation.(Table 1).
Table 1. Stool examination of the pupils I n f e s t a t i o n Number of
Positive Single % Mixed %
469 95 20.3 374 79.7
In this study we found that the prevalence of A.lumbricoides 22.7% ; Trichuris trichiura 68.2% and Hookworm 47.5% (Table 2).
Table 2. Prevalence of soil transmitted helminthiasis
A. Lumnricoides T. Trichiura Hookworm
Number of
examined No. (+) % No. (+) % No. (+) %
541 123 22.7 369 68.2 257 47.5
Table 3. Occupational status of the father
Occupation Number Persentage
Laborer/Farmer
This table shown us the occupation of father was laborer/farmer 55% and 24% was entrepreneur. Government employee only 8% (table 3)
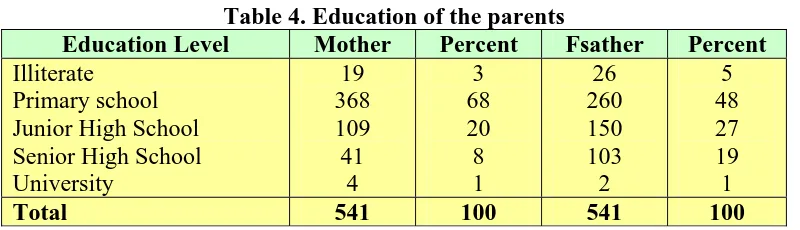
Table 4. Education of the parents
Education Level Mother Percent Fsather Percent
Illiterate Primary school Junior High School Senior High School University
Table 5. Relation between nutritional status and parasitic infestation Parasitic Infestation
Nutritional Status
Parasitic infestations in the wellnourished children and mild/moderate malnutrition didn't differ, that is 86.3% dan 88.6% (Table 5).
Table 6. Relation between gender and parasitic infestations Parasitic infestations
No relationship between gender and parasitic infestation (p>0.05).(Table 6)
Table 7. Relation between age and parastic infestations Parasitic infestations
No significant difference between age and parasitic infestation in this study (p>0.05). (Table 7)
Marwi MA (1979) have been found that the sensititivy of Harada-Mori's technic was 85.57% and Kobayashi et al in 1966 was 79.6%19. It means that the sensitivity of HardMori's technic more better than Kato-Katz's technic.
CONCLUSIONS
Modified Harada-Mori technique is still better than modified Kato-Katz thick smear, as a diagnostic tool for hookworm infestations.
REFERENCES
Coulad JP. Traitment des nematodoses. Ann Soc Belge Med Trop, 1983;63:5-20.
Fain A. Les maladies parasitaires en Europe. Ann Sac Belge Med Trop, 1980;60:3-26.
Gatti F., Vanderick K., Parent M., Bulihereme J., et Vendepitte J. Treatment of roundworm infestation in African children with a single dose of tetramisole (R.8299). Ann Sac Belge Med Trop, 1969; 49 :51-62.
Kaba AS., Luvwezo M., Nzuzi K et Thiepont D. Le traitment anti-helminthique d'enfants d'age scolaire au Zaire. Ann Soc Belge Med Trop, 1978 ; 58 : 241-249.
Kadio A., Moreau J., Gazin J et Caudet H. L'albendazole (Zentel) dans le Traitment de l'ankylostomiase en Cote d'Ivoire.
Krubwa F., Gatti F., Lontie M., Nguete K., Vendepitte Jet Thiepont D. Administration trimestrielle de mebendazole en milIeu scolaire suburbain. Med Trop, 1975;34:679-687.
Nwosu ABC. Intestinal helminthiases in Nigeria : Epidemiology, Infection dynamics and control strategies. Med Afr noire, 1982 ; 29 : 4449 - 53.
Vendepitte J. Helminthologie mediale. P.U.Z.Kinsha sa, 1973:45
Clarke MD., Cross JH., Carney WP., Bechnee WM., Sri Oemijati., Partono F., Hudojo., Arbain J. and Noerhayati S. A parasitological survey in the Jogyakarta area of central Java. Indonesia. SEA J Trop Med Pub Hlth, 1973 ; 4 : 195.
Carney WP., Atmosoedjono S., Sajidiman Hand Arbain J. Intestinal parasites and malaria in Sukamenanti Pasaman Regency West Sumatera. Bull Hlth Studies Indonesia,1974;2:61.
Cross JH., Clarke MD., Durfee PT., Irving GS., Taylor J., Partono F., Arbain J., Hudojo and Sri oemijati. Parasitological survey and seroepidemiology of amoebiasis in South Kalimntan (Borneo), Indonesia. SEA J Trop Med Pub Hlth,1975;6:52.
Rasidi R., Margono SS., Simanjuntak GM and Koesharjono C. Intestinal parasites in villages of Bali. Maj Kedokt Indon; 1979;29:3.
Abadi K., Tjowandi F., Sasabone P., Rambulangi J, Djajakusli L and Haerani T. Survey on insidence the anthelmintic in a mass treatment. Department of Parasitology, Faculty of Medicine, Hasanuddin university , Ujung Pandang, Sulawesi (in Indonesian), 197
Abidin SAN. and Rased R. Treatment of intestinal nematodes using single dose 500 mg mebendazole, Medika, 1990;33 :192-197.
Kazura JW and Mahmoud ADF. Helminths in Nelson Textbook of Pediatrics. Edited by Behrman RE, Vaughan VC, Nelson WE. 13th Eds. WB.Sauders Company, 1987:739-743.
Sasa M. Diagnosis of hookworm and Strongyloides infections by Faecal culture method.
Gilles HM. Hookworm infection and anemia in Clinical Tropical Diseases, edited by Maegraith B, 8th Eds. Blackwell Scientific publications, 1984:178-188.