PRETES 2
dr. Syah Rini Sp.OG, M.Kes
Pendahuluan
Intrauterine Growth Restriction (IUGR)
Kegagalan janin untuk mencapai perkembangan yang sesuai potensinya
Saat ini, diagnosis berdasarkan EFW (Estimated Fetal Weight) di bawah
persentil 10
Sensitivitas kurang
(gagal terdiagnosis bila ada hambatan perkembangan, namun EFW janin
tidak kurang dari persentil 10) Luaran perinatal buruk
Penegakan diagnosis merupakan hal yang penting
Mencegah Intrauterine Fetal Death (IUFD), cedera otak perinatal dan fetal distress intrapartum yang berat
Managemen untuk monitoring dan rekomendasi usia saat
persalinan
Fase Pertumbuhan
Hiperplasia
• 0-16 minggu
• Mitosis cepat
• Jumlah DNA
Hiperplasia &
Hipertrofi
• 17-32 minggu
• Mitosis
• Ukuran sel
Hipertrofi
• >32 minggu
• Ukuran sel , deposisi lemak, massa otot dan jaringan ikat
15 minggu 5 gram/hari
24 minggu 10-20 gram/hari
34 minggu 30- 35 gram/hari
Fase Pertumbuhan
Peningkatan berat janin (gram/hari) berdasarkan usia
kehamilan
garis hitam: rata-rata garis biru: ± standar deviasi
Faktor Risiko dan Etiologi
Faktor Risiko yang mempengaruhi pertumbuhan janin terhambat meliputi
potensi abnormalitas pada ibu, janin, dan plasenta
Identifikasi
perkembangan janin
↓
Sonography
Paling umum dilakukan
Femur Length
Biparietal diameter
Head circumference
Abdominal circumference
Estimated Fetal Weight
(EFW)
IUGR vs SGA
Janin Kecil
IUGR
Intrauterine Growth Restriction
SGA
Small for Gestational Age
Janin yang kecil, dengan risiko luaran perinatal lebih buruk dibandingkan janin yang tumbuh
normal
Terdapat redistribusi
hemodinamik sebagai respon adaptasi janin terhadap kondisi
undernutrition, hipoksia atau gangguan (insufiseiensi) plasenta
Janin yang kecil, dengan luaran perinatal yang sama baik seperti
janin yang tumbuh normal Tidak terdapat tanda-tanda respon adaptasi janin terhadap perubahan pada lingkungannya juga mempunyai risiko kelainan
perinatal dan neurodevelopmental
• 1. Which of the
following is a risk factor for poor fetal growth?
• a. Malaria
• b. Tuberculosis
• c. Cytomegalovirus
• d. All of the above
• 2. Which of the following statements is
closely associated with the characteristics of human fetal growth?
• a. Need a narrow pelvis to walk upright
• b. A large head is needed for a large brain
• c. The ability to growth restrict may be adaptive
• d. All of the above
• 3. How is symmetrical versus asymmetrical growth restriction differentiated?
• a. Symmetrically growth restricted fetuses were proportionately small.
• b. The abdominal circumference to head circumference ratio is used to differentiate between the two.
• c. Asymmetrically growth restricted fetuses had a disproportionately lagging head
compared with
• abdominal growth.
• d. All of the above
• 4. Which of the following statements is true regarding brain sparing and growth restriction?
• a. Brain sparing is restricted to symmetrically growth restricted fetuses.
• b. With limited nutrients, there is preferential shunting of oxygen and nutrients to the brain.
• c. During the last 12 weeks of growth in the growth restricted infant, brain sparing is demonstrated by
• a brain-to-liver weight ratio of 3:1 instead of the normal 2:1.
• d. All of the above
• 5. Growing evidence suggests that fetal growth restriction affects organ development,
especially which of the following?
• a. Brain
• b. Heart
• c. Kidney
• d. Thyroid
• 6. Risk factors for impaired fetal growth are divided into mother, fetus, and placenta. Which of the following is a common risk factor to all three sources?
• a. Infection
• b. Drugs and teratogens
• c. Genetic abnormalities
• d. Maternal medical conditions
• 7. Which of the following markers is associated
with fetal overgrowth?
• a. IGF-1
• b. Hyperglycemia
• c. Hyperinsulinemia
• d. All of the above
• 8. What risk factors are associated with fetal growth
restriction in
women with pre- gestational
diabetes?
• a. Maternal vascular disease
• b. Congenital malformations
• c. Worsening White classification
• d. All of the above
• 9. Compared to women who do not undergo psychosocial risk factor screening during
pregnancy, those that do have which of the following?
• a. Lower preterm birth rates
• b. More appropriate interventions
• c. Lower rates of low-birthweight newborns
• d. All of the above
• 10. The presence of which of the following vascular diseases during pregnancy leads to the highest
perinatal morbidity rates?
• a. Class F diabetes
• b. Valvular heart disease
• c. Ischemic heart disease
• d. Chronic hypertension
Kehamilan multifetal meningkat sebanyak 3% pada populasi dunia. Persalinan preterm merupakan masalah utama dari kehamilan multifetal, global survey dari WHO menyatakan 35.2 % kehamilan multifetal berakhir dengan persalinan preterm (Fallis, 2013; Wei, 2016)
PENDAHULUAN
Kehamilan multifetal merupakan hasil dari 2 atau lebih kejadian fertilisasi, fertilisasi tunggal diikuti pembelahan
”erroneous´ dari zigot, atau kombinasi dari keduanya (Cunningham, 2018)
FAKTOR RISIKO
• 3,5% pada wanita kulit hitam, 3 % pada wanita kulit putih.
Wanita Hispanik, Asia dan Amerika kemungkinanya lebih rendah daripada wanita kulit putih.
Ras
• Kejadian kembar dizigot meningkat pada usia 15-37 tahun
Usia saat kehamilan
• Kemungkinan meningkat 8x lipat saat paritas ≤4 dan 20x lipat saat paritas ≥5 (Olusanya,2012)
Jumlah paritas
• Riwayat kembar dari ibu lebih berpengaruh daripada riwayat kembar dari ayah
Hereditas
• Beberapa penelitian menunjukkan wanita yang mendapat asam folat memiliki prevalensi yang lebih tinggi. Pada World War II di eropa saat pemenuhan nutrisi bagi wanita hamil lebih sulit tercatat penurunan angka kehamilan kembar
Nutrisi
• Peningkatan kelahiran kembar berkaitan dengan pelepasan FSH hipofisis yang berlebihan sebagai respons terhadap penurunan umpan balik negatif dari kegagalan impending ovarium
Gonadotropin Pituari
• Induksi ovulasi dengan FSH plus human chorionic gonadotropin (hCG) atau klomifen sitrat meningkatkan kemungkinan ovulasi bersamaan.
Terapi Infertilitas
Dizigotik vs Monozigotik
Dizigotik
Lebih sering
Dipengaruhi kadar FSH (geografi, ras, multipara, usia,
kontrasepsi)
Selalu dikorionik
Monozigotik
Jarang (3.5-4/1000 kelahiran)
Paling dipengaruhi genetik
Korionisitas tergantung kapan
membelah
(Cunningham et al, 2018) (Basiri et al, 2019)
KLASIFIKASI
DIAMNION
DICHORION
23
DIAGNOSIS MULTIFETAL
Evaluasi Klinis Sonograf
• Pengukuran TFU. Memantau pertumbuhan janin & volume cairan amnion. Pada uk 20-30 minggu dapat > 5 cm daripada kehamilan tunggal
• Palpasi. Menentukan bagian janin pada trimester ketiga, penyulit : posisi janin saling tumpang tindih, ibu dengan obesitas dan hidramnion.
• Pemeriksaan DJJ, dengan alat Doppler dapat dibedakan jika letak jantung janin cukup berjauhan
• Tidak disarankan diagnosa
multifetal hanya
menggunakan 1 kriteria
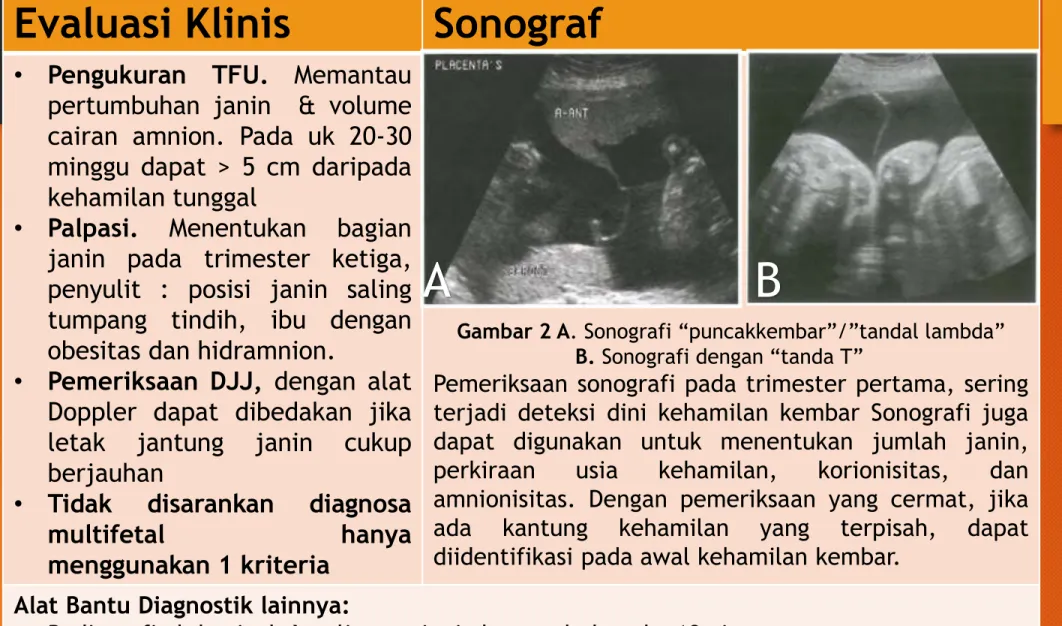
Gambar 2 A. Sonografi “puncakkembar”/”tandal lambda”
B. Sonografi dengan “tanda T”
Pemeriksaan sonografi pada trimester pertama, sering terjadi deteksi dini kehamilan kembar Sonografi juga dapat digunakan untuk menentukan jumlah janin, perkiraan usia kehamilan, korionisitas, dan amnionisitas. Dengan pemeriksaan yang cermat, jika ada kantung kehamilan yang terpisah, dapat diidentifikasi pada awal kehamilan kembar.
Alat Bantu Diagnostik lainnya:
• Radiografi abdominal sulit saat janin bergerak dan uk <18minggu
• Magnetic Resonannce Imaging patologi kembar yang lebih detail
• Kadar β-hCG dan maternal serum levels of alpha-fetoprotein (MSAFP) meningkat
A B
• Evaluasi USG perkiraan usia kehamilan, menentukan korionisitas dan screening Down’s syndrome
Menentukan usia kehamilan dan korionisitas
• Lebih beresiko anemia rutin evaluasi as folat/zat besi
Diet and Nutrisi
Perawatan spesialistik
• Skrining down syndrome saat CRL : 45 mm - 84 mm (pada usia kehamilan : 11 – 13+6 minggu)
• Screening kombinasi : nuchal translucency, β hCG , pregnancy associated plasma protein A)
• Monitoring untuk IUGR
Komplikasi Janin
SKRINING
Usia kehamilan 16-17, 19-20, dan 21-22 minggu
untuk skrining TTTS dan TAPS serta skrining jantung sebagai bagian dari skrining anatomi lengkap pada minggu ke 18-19 minggu atau pada
minggu ke 21-22.
USG pada usia kehamilan 11+0 minggu hingga 13+6 minggu (CRL 45-84 mm)
berfungsi untuk menilai viabilitas janin, usia kehamilan dan korionisitas, serta melihat adanya
malformasi kongenital mayor
Jika tidak terdapat kelainan dilanjutkan pemeriksaan pertumbuhan pada minggu
ke 24, 28, 32 dan 34
PILIHAN PERSALINAN
Direncanakan sejak UK 24 - 28 minggu (tempat, waktu, metode, dan resiko persalinan)
- Tanpa komplikasi uncomplicated triplet pregnancies elektif UK 35 minggu (setelah + kortikosteroid)
Persiapan standar untuk pelaksanaan persalinan + pertimbangan khusus untuk wanita dengan kehamilan multifetal
Posisi dan presentasi janin paling baik dikonfirmasi secara sonografi
Gambar 3. Macam-macam presentasi janin pada kehamilan kembar
Sumber: https://obgynkey.com/multiple-pregnancy-and-other-antenatal-complications/
2016 Royal College of Obstetricians and Gynaecologists
Christopher D, Robinson BK, Peaceman AM. An evidence-based approach to determining route of delivery for twin gestations.
Rev Obstet Gynecol. 2011;4(3-4):109-116.
Gambar 4. Alur pemilihan persalinan pada kehamilan kembar (Christoper, 2011)
PILIHAN PERSALINAN
MATERNAL
Persalinan preterm (35.2%)
( Jun Wei, 2016)
Hipertensi dalam kehamilan 2.5 -2.8 kali
(Devine and Malone, 2004)
Diabetes dalam kehamilan
2.2 kali
(Rauh-Hain et al., 2009).
AFLP
7.1% hingga 28.6%
(Minakami et al., 2014).
Anemia
(multifetal triplet, 70%)
(Devine and Malone, 2004).
Cholelitiasis 0.4% - 5.5%
(Rissanen et al., 2019)
KOMPLIKASI
(ACOG, 2016)
KOMPLIKASI
Preterm Delivery
Deteksi
• Pada pasien asimptomatik tidak dianjurkan melakukan tindakan intervensi yang bertujuan untuk skrining risiko preterm
• Pada pasien simtomatik dapat dilakukan pengukuran panjang serviks dan skrining fetal fibronectin sebagai bantuan untuk prediksi risiko kelahiran preterm. Panjang serviks 25mm adalah cut-off paling sering digunakan pada trimester kedua
Pencegahan • Belum ada Tindakan intervensi yang direkomendasikan untuk memprolong masa kehamilan
Manajemen
• Tokolitik dapat diberikan untuk memperpanjang masa kehamilan jangka pendek
• Pemberian kortikosteroid antenatal untuk wanita hamil usia 24-34 minggu mengurangi insiden kematian neonatal karena distres pernapasan
• Pemberian magnesium sulfat prenatal dapat dilakukan untuk mengurangi terjadinya cerebral palsy
FETAL
Gambar 2. Overview insidensi komplikasi kehamilan ganda (Cunningham, 2014)
KOMPLIKASI
Dichorion
Diamnion
Monochorion Diamnion
Monochorion Monoamnion
TTTS Rare 15% 2-6%
TAPS - Up to 5 % -
TRAP - 1% 1%
sIUGR 11.6% 12% -
Tabel 1. Insidensi komplikasi fetal pada kehamilan Multifetal (Rauh-Hain et al., 2009; Anca et al., 2015; Buyukkaya, Tekbas and Buyukkaya, 2015; Johnson, 2015; K.Behavkova, 2016; Lanna et al., 2019; Antonakopoulos et al., 2020; Gleeson et al., 2020)
KOMPLIKASI
Twin to Twin Trnasfussion syndrome
Mempengaruhi 15% dari kehamilan multifetal monochorionic.
FETAL
• Treament of choice adalah ablasi laser pada quintero stage II (Rekomendasi: A)
• Konservatif management dilakukan pada quintero stage I (Rekomendasi B)
• Amnioreduction bertahan sebelum usia kehamilan 26 minggu (Rekomedasi A) (Khalil et al., 2016)
MANAGEMENT
KOMPLIKASI
Twin Anemia – Polycyteamia Sequence (TAPS)
Mempengaruhi 2% dari kehamilan multifetal dan 13% setelah mendapatkan terapi ablasi laser
FETAL
Pilihan terapi pada TAPS bergantung kasus per kasus. Terapi paling umum adalah konservatif, early delivery, ablasi laser, transfusi intrauterine, partial exchange transfusion (Evidence Level 3) (Khalil et al., 2016).
MANAGEMENT
KOMPLIKASI
Twin Reversed Arterial PerfusionSequence (TRAPS) FETAL
Terapi utama dari TRAPS adalah discontinuation transfusion dari janin acardiac, dengan cara ligasi tali pusat dari janin acardiac (Evidence Level 3).
(Khalil et al., 2016)
Twin Reverse Arterial Perfussion (TRAP) terjadi pada 1% kehamilan multifetal dengan janin kedua acardiac.
MANAGEMENT
KOMPLIKASI
Selective Intra Uterine Growth Restriction
FETAL
Terminasi merupakan pilihan utama dimana bila termasuk dalam tipe I direkomendasikan pada usia kehamilan 34-36 minggu, sedangkan pada tipe II dan III disarankan dilakukan terminasi pada usia kehamilan 32 minggu
MANAGEMENT
• sFGR, secara konvensional, didefinisikan sebagai suatu kondisi di mana satu janin memiliki EFW <10 percentile dan diskrepansi EFW dengan kembarannya > 25%
• Terjadi pada 10-15% kehamilan multifetal
• Tipe I, waveform doppler arteri umbilikalis terdapat positive end-diastolic flow
• Tipe II, terdapat absent or reversed end- diastolic flow (AREDF).
• Tipe III, terdapat pola AREDF yang memebntuk siklus/intermittent
11. All except which of the following complications are increased in multifetal
gestations?
• a. Preeclampsia
• b. Hysterectomy
• c. Maternal death
• d. Postterm delivery
• 12. Which of the following mechanisms may result in monozygotic twins being discordant for malformations or traits?
• a. Prezygotic mutation
• b. Variable expression of the same genetic disease
• c. Skewed lyonization in male fetuses with differential expression of X-linked traits or diseases
• d. All of the above
• 13. A 37-year-old G1 comes to establish prenatal care with you
after being discharged from her reproductive endocrinologist. This pregnancy was conceived via single embryo transfer in vitro
fertilization. Which one of the following is true regarding her situation?
• a. Assisted reproductive technology increases the incidence of monozygotic twins two- to fivefold.
• b. If a single zygote splits 8 days post fertilization, a monochorionic diamnionic twin gestation results.
• c. Because this pregnancy is known to have begun with one embryo, you can be certain that she will have monochorionic twins, but amnionicity depends on timing of split.
• d. All of the above
• 14. A 29-year-old G1P1 conceived dichorionic twins via gonadotropin
stimulation and intrauterine insemination (IUI) with her husband’s semen. Her blood type is O-negative, so prior to receiving anti-D immune globulin the neonates’
blood type is assessed. One neonate is A- positive and the other is O-negative. Her husband is A-positive. This finding can be explained to the parents by describing which of the following phenomena?
• a. Superfetation
• b. Superfecundation
• c. This is not atypical for dichorionic twins
• d. This cannot be explained without alleging infidelity or poor technique by her reproductive endocrinologist’s office.
• 15. Which of the following factors increases the risk for monozygotic twinning?
• a. Maternal age
• b. Increased parity
• c. Race and family history
• d. None of the above
• 16. Which hormone is the most likely underlying cause of increased twinning seen in some racial and ethnic groups?
• a. Estrogen
• b. Progesterone
• c. Luteinizing hormone
• d. Follicle-stimulating hormone
• 17. Which of the following statements regarding
atypical twinning is not true?
• a. Monochorionic twins are never dizygotic.
• b. Twins of opposite sex are not always dizygotic.
• c. Monochorionic twins are not always the same sex.
• d. None of the above is true
• 18. Maternal physiological
adaptation to twin pregnancy in comparison to a singleton
pregnancy is accurately described in which of the following
statements?
• a. Cardiac output increases 40%
above that of a woman carrying a singleton fetus.
• b. Blood volume expansion
averages 70%, which is greater than the 40–50% seen in women carrying
• a singleton.
• c. The increased cardiac output in twin gestation is primarily due to increased stroke volume rather than increased heart rate.
• d. All of the above
• 19. It is well known that miscarriage is more likely with a multifetal
gestation. Which of the following statements is not true?
• a. Before 12 weeks, one or more
fetuses are lost in about 50% of initial triplet pregnancies.
• b. Twins conceived via assisted
reproductive techniques are at greater risk for spontaneous loss.
• c. Spontaneous loss of a cotwin before the second trimester occurs in 10–40%
of all twin gestations.
• d. None of the above is true.
• 20. A 34-year-old G2P1 at 12 weeks’ gestation presents to discuss aneuploidy
screening. This pregnancy started out with dichorionic twins, but spontaneously reduced to singleton at 7–8 weeks’ gestation. Which of the following is the most appropriate?
• a. First-trimester screening is not recommended.
• b. Since the cotwin demise occurred prior to 9 weeks, routine first-trimester screening is not affected and remains a valid option.
• c. Since it has been at least 4 weeks since cotwin demise, routine first- trimester screening is not affected and remains a valid option.
• d. Second-trimester maternal serum alpha fetoprotein will be falsely elevated, so a detailed anatomy ultrasound is recommended to assess for neural tube
defect.
• 21. Characteristically,
menopausal transition begins with a variable period of
menstrual cycle irregularity and extends to 1 year after permanent cessation of
menses. The menopause
transition typically spans how many years?
• a. 1 to 2 years
• b. 2 to 4 years
• c. 4 to 7 years
• d. 7 to 10 years
• 22. Premature ovarian failure is associated with a persistently elevated follicle-stimulating
hormone (FSH) level and is further de ned as cessation of menses before what age?
• a. 35 years
• b. 40 years
• c. 45 years
• d. 51 years
• 23. Several factors can alter ovarian aging. Which of the following is
LEAST likely to shift menopause to an earlier age?
• a. Smoking
• b. Chemotherapy
• c. Pelvic radiation
• d. Oral contraceptive pills
• 24. During menopausal transition, erratic
fluctuations in female reproductive hormones lead to an array of physical and psychological symptoms. These symptoms include all of the following EXCEPT:
• a. Headache
• b. Poor memory
• c. Vision changes
• d. Urinary incontinence
• 25. During the reproductive life of a woman, gonadotropin- releasing hormone is released in a pulsatile fashion from which of the
following?
• a. Corpus lutea
• b. Ovarian follicles
• c. Pituitary gonadotrophs
• d. Arcuate nucleus of the hypothalamus