COMPLICATION OF USING LATTISSIMUS DORSI MYOCUTANEOUS FLAP ON BREAST RECONSTRUCTION SURGERY: A CASE REPORT
Dewi Prima Christian, Putu Anda Tusta Adiputra, W. Steven Chr.
Subdivision of Surgical Oncology, Departement of Surgery Faculty of Medicine, Udayana University – RSUP Sanglah
Denpasar FOREWARD
Extensive clinical experience with the LDMF has documented the safety of the procedure of breast reconstruction surgery. The flap has a good and vigorous blood supply and can be used with minimal risk of flap necrosis, even in the smokers, diabetics, and patient with medical illness. Significant flap necrosis is very unusual and is nearly always associated either recognized of unrecognized injury to the vascular pedicle, as when the thoracodorsalis artery has been ligated during the original mastectomy. Partial flap necrosis has been noted in up to 7 % of cases.
CASE REPORT
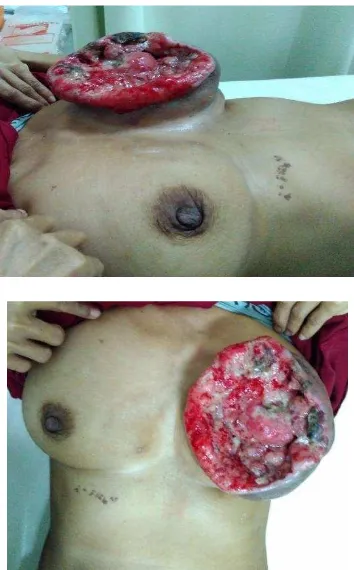
A 53 year old woman, suffered with a huge tumor on her left breast. Clinical investigations and on biopsy examination was benign phyloides of the breast. Mastectomy was done and immediate LDMF underwent to reconstruct the leaving defect of surgery. On the second day after surgery LDMF was noted partial necrosis and tend to totally necrosis.
CONCLUSION
LDMF is common procedure to reconstruct the leaving defect after mastectomy. The cause of necrosis may due to technical error and impact to vascular compromise. The vascular injury and thrombosis during and after surgery may be responsible for the event of flap necrosis.
Key words: Mastectomy, LDMF, Necrosis, Vascular injury
COMPLICATION OF USING LATTISSIMUS DORSI MYOCUTANEOUS FLAP ON BREAST RECONSTRUCTION SURGERY: A CASE REPORT
Dewi Prima Christian, Putu Anda Tusta Adiputra, W. Steven Chr.
Subdivision of Surgical Oncology, Departement of Surgery Faculty of Medicine, Udayana University – RSUP Sanglah
Denpasar
FOREWARD
Reconstructive surgery in the cancer patient endeavors to restore form and function following ablative surgery (Jules A., et al, 2006)Breast reconstruction is an important component of breast cancer management and should be a safe procedure of appropriate complexity for the patient. The use of the latissimus dorsi (LD) myocutaneous flap as a primary method of reconstruction has declined since the 1970s and originally described by Tansini in 1906 for use as an axial musculocutaneous flap to cover mastectomy defect ( Danies C., 2006)
Reconstructive surgery of the breast cancer can be performed in the immediate or delayed setting (Jules A., et al , 2006) The timing of reconstructive surgery is influenced by the tumor pathology, extent of resection, adjuvant therapy, surgical expertise, and patient preference. Successful reconstructive surgery achieves restoration of function and form with minimal donor site deformity and consequent enhancement of quality of life (Jules A., 2006)
Extensive clinical experience with the LDMF has documented the safety of the procedure of breast reconstruction surgery
(Danies C., 2006) The flap has a good and vigorous blood supply and can be used with minimal risk of flap necrosis, even in the smokers, diabetics, and patient with medical illness. Significant flap necrosis is very unusual and is nearly always associated either recognized of unrecognized injury to
the vascular pedicle, as when the
thoracodorsalis artery has been ligated during the original mastectomy (Danies C., 2006, Mendelson BC., 1983, De Mey A., et al. 1991). Partial flap necrosis has been noted in up to 7 % of cases (Danies C., 2006, De Mey A., et al. 1991, Hokin JAB, Silfverskiold KL, 1987, Barnett GR, et al, 1992).
Patient and Method
LDMF underwent to reconstruct the leaving defect of surgery.
Figure 1a and 1b . Clinical figure of patient with benign phyloide on the left breast.
On the first day after surgery LDMF was noted vascular compromised and there is sign of the tissue necrosis at the end of the flap. The skin color was changed become blackish. Re explore of the flap was done at the second day to evaluate the extension of the vascular compromised. There is no significant obstacle of the vascular bundle that may cause diminished of the blood supply to the flap. Debrided of the skin and fat tissue was done and performing the needle puncture decompressing of the skin island of the flap to decrease the tension of the tissue. The next day the whole skin of the flap become darker and tend to be total
necrosis. Finally, the entire skin, fat excised and just leave the muscle alone, and covered with skin graft. The island of the flap was harvested too extend, almost at the end of the muscle.
Figure 2. Mastectomy defect during
operation.
Figure 3. Latissimus Dorsi myocutaneous flap (LDMF) after surgery.
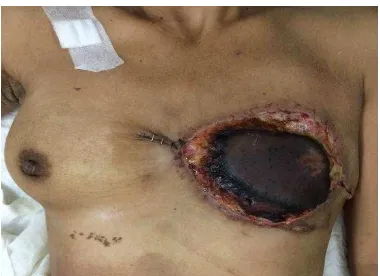
Figure 5. Post operation day 1, necrosis at the end of the flap and the skin color was change become blackish.
Figure 6. Necrotic flap getting worse in a couple of day and more dark than before.
Discussion
The Latissimus Dorsi muscle is the largest and most superficial of the muscles of the posterior chest wall. It is a broad, flat muscle that extends from a wide area of the origin over the posterolateral thorax. The blood supply to the Latissimus Dorsi muscle is constant arises from thoracodorsalis vessel as the branch of axillary vessel.
Although the LDMF procedure is safe on the breast reconstructive surgery but the surgeon still has awareness of the arising of complication at any time. Knowing the anatomy of donor site like LD component is very important to finish reconstruction successfully. Accurate preoperative marking are vital to properly position the skin island and should always be made with the patient upright (Jules A., et al, 2006) Extensive clinical experience with the LDMF has documented the safety of the procedure of breast reconstruction surgery. The flap has a good and vigorous blood supply and can be used with minimal risk of flap necrosis, even in the smokers, diabetics, and patient with medical illness.
Breast reconstructive surgery
Our patient revealed the vascular compromised on the first day after reconstructive surgery, and become worst on the following day. The plan of re- exploration of the flap immediately after it
recognized the present of vascular
compromised. Trying to decompression of the tension tissue with needle, but it did not improve. The next day the necrosis of the skin island of LDMF was excised and skin graft was done.
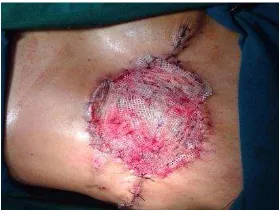
Figure 7a. During second operation, necrotomy of necrotic flap and debridement of wound defect.
Figure 7b. Skin graft on the defect.
Figure 7c. Donor site from left femoral .
Conclusion
LDMF is common procedure to reconstruct the leaving defect after mastectomy. The cause of necrosis may due to technical error and impact to vascular compromise. The vascular injury and thrombosis during and after surgery may be responsible for the event of flap necrosis. The LDMF was taken too extent, and may cause diminished of blood supply of the flap tissue. Planning prior reconstructive surgery is very important to all surgeons to make all
things successfully. Discipline and
experience of the surgeon on reconstructive surgery may become more important than just doing the harvest.
References
Barnett GR, Gianoutsos MP, 1996. The LD added fat plaf for natural tissue breast Reconstruction: Report of 15 cases. Plast Reconst Surg; 97:63
Bostwick J, Nahai F, Wallace JG, et al.1979. Sixty Lattissimus Dorsi Flaps. Plast Reconst Surg; 63:31
Danies C. Hammond. 2006. Latissimus
Reconstruction. In : Surgery of the Breast. 2nd. Scott L Spear. Lippincott Williams and Wilkins:1: 601
De Mey A., Lejour M., Declety A., et al. 1991. Late Result and current indication on LD breast Reconstruction. Br J Plast Surg; 44:1
Gabriel N. Hortobagyi, Sonja Eva
Singletary, and Eric A Storm, 2010. Locally Advanced Breast Cancer. In : Disease of the Breast. 4th Ed. Ed by Jay R. Harris, Merc E. Lippman, Monica Morrow, C.Kent Osborne.
Lippincott Williams and Wilkins.
Philadephia. 752
Geoffrey G. Hallock. 2009. In : Flap and
Reconstructive Surgery. Wei-Mardini.
Elsevier Inc: 3:16
Hokin JAB, Silfverskiold KL, 1987. Breast Reconstruction without an Implant: Result and complication using an extended LD flap. Plast Reconst Surg; 79-58
Jules A. Feledy Jr., Mathew M. Hanasono, Geoffrey L. Robb. 2006. Reconstructive Surgery in the Cancer Patient. MD Anderson Surgical Oncology Handbook. 4th Ed. Lippincoot Williams and Wilkins.: 24
Mendelson BC., 1983. Lattissimus Dorsi Breast Reconstruction and Result. Br J Surg; 70: 45
Moore TS, Farrell LD, 1992. Lattissimus Dorsi Myocutaneous Flap for Breast Reconstruction: Longterm Result. Plast Reconstr Surg.; 89: 666